How gastric bypass surgery works and why it helps with weight loss
March 9, 2026
By: Mark Choh, MD
Categories: Bariatrics, Bariatric Surgery, Bariatric and Metabolic Surgery
Gastric bypass surgery is one of the most effective and well‑studied procedures for helping people achieve significant, lasting weight loss. For individuals struggling with obesity and related health conditions, it can be a life‑changing tool that improves overall health, reduces comorbid disease risk and supports long‑term well‑being. Still, many people have questions about how the surgery works, who qualifies and what life looks like afterward.
What is gastric bypass surgery?
Gastric bypass surgery, also known as Roux-en-Y gastric bypass, is a type of bariatric procedure that changes the anatomy of the upper gastrointestinal tract. The stomach is separated into two sections, one of which is much smaller than the other. This smaller section, known as a pouch, is the size of an egg and is then connected to your small intestine, creating a new pathway for digestion and absorption of food.
The creation of the small pouch, combined with the re-routed intestines creates a powerful combination of restriction of food intake, malabsorption of ingested fat and carbohydrates and metabolic change in digestive hormones that help control hunger, appetite and fullness to support weight loss and metabolic health.
“By bypassing a segment of small intestine, gastric bypass shifts gut hormones in a way that helps with insulin resistance and blood‑sugar control, one reason it can outperform medications for some patients,” says Mark Choh, MD, bariatric surgeon at Loyola Medicine.
Who is a good candidate for weight loss surgery?
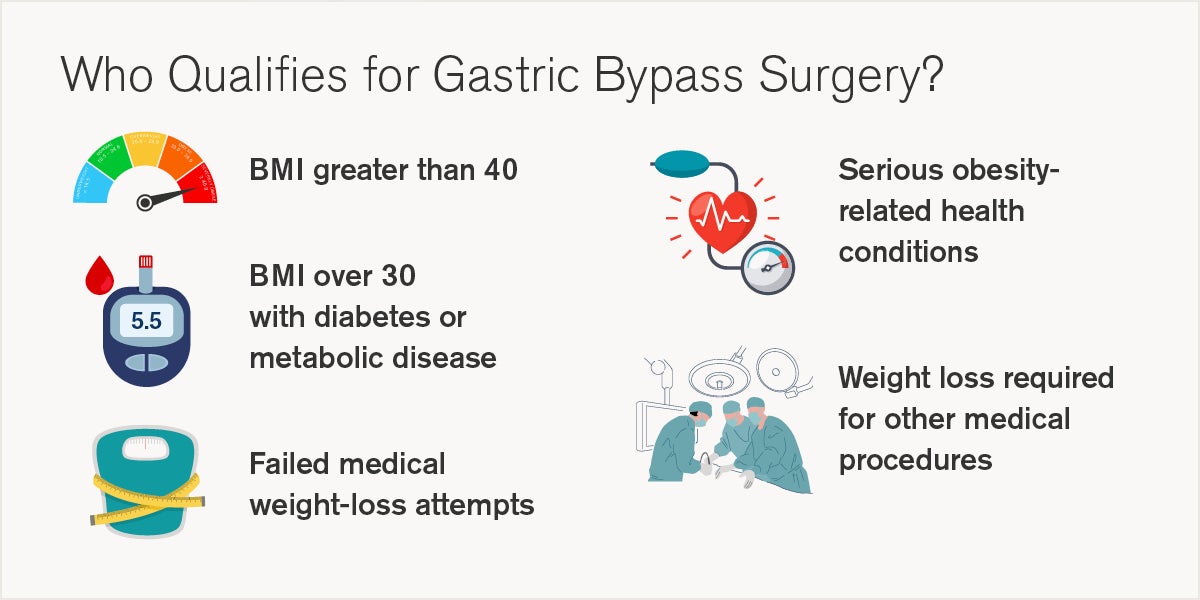
Bariatric procedures help treat obesity in individuals, defined as someone having a body mass index (BMI) greater than 30. The general guideline for candidacy of gastric bypass, and other weight loss surgeries, is a BMI greater than 40 or if your BMI is 35 and you have comorbid conditions that are affected by your weight, such as diabetes, sleep apnea, or hypertension.
Benefits of gastric bypass (Roux-en-Y) surgery
The main benefit of gastric bypass surgery is weight loss. Additional benefits are more indirect. Because obesity can weaken the body’s immune system, increasing the risk for many other diseases and conditions, the loss of excess weight can cause the remission of various obesity-related diseases, such as:
- Type 2 diabetes
- Hypertension
- Obstructive sleep apnea
- Dyslipidemia, an imbalance of lipids (fats) in the blood
- Cardiovascular disease
“For patients with type 2 diabetes, especially severe diabetes, gastric bypass is often a better choice than sleeve gastrectomy if remission is the goal. It’s also a strong option for people with significant acid reflux,” says Dr. Choh.
Common concerns about gastric bypass surgery
Like any major surgery, there are standard risks associated with gastric bypass. Many of these risks are the same as with any operation, like bleeding, infections, blood clots and cardiac complications. There are also more bariatric-specific risks that include possible leaks and other similar infections, as well as longer term risks such as pouch ulcers or bowel obstructions. However, these risks don't outweigh the risks of severe obesity if left untreated. Because gastric bypass has become such a routinely performed procedure and surgical methods continue to advance, the likelihood of experiencing a major complication is now exceptionally low.
Recovery is also minimal, with patients staying in the hospital for one to two days and needing no additional care at home. They can return to work within a couple of weeks and start exercising again within a couple of months.
Long-term bariatric care for a healthier future
For a number of reasons, we strongly recommend long-term follow-up with your bariatric surgery team after surgery. Because the procedure makes it more difficult to absorb nutrients, we recommend each bariatric surgery patient to take supplements for the rest of their life. By following up, we can monitor your system for any potential vitamin and nutrient deficiencies and catch them early before they become a significant issue.
In addition, the long term follow-up helps keep you engaged and motivated, helps pick up on small problems before they become bigger ones and can help stave off weight regain if it starts to happen years after surgery.
However, patients who stick to a permanent, healthy diet, get regular exercise, maintain follow-up appointments and stick to supplementation will lose significant weight and live a normal life.
“We treat obesity as a chronic disease. Surgery helps you reach your goals. However, maintaining them requires work, like meal planning, physical activity and monitoring. If weight starts to creep up, early follow‑up lets us course‑correct,” says Dr. Choh.
Misconceptions about gastric bypass surgery
Like many bariatric surgeries, there are many misconceptions about gastric bypass surgery that can stop patients from getting the help they need.
“These operations are extremely safe. The risk of major or even minor complications is very low, and the vast majority of patients do very well. The most common regret I hear is that patients wish they had done it sooner,” says Dr. Choh.
Myth #1: Bariatric surgery is the easy way out
While gastric bypass surgery can help patients lose a significant amount of weight and keep it off, it still requires permanent lifestyle changes, long-term commitments and significant behavior changes to keep the weight off and improve your health outcomes.
Myth #2: I’ll regain all the weight
While it's true that on average, patients regain 15% of their weight loss after 10 years, the vast majority maintain significant weight loss and health benefits. Patients that commit to post-surgery lifestyle changes have a much greater chance at keeping the pounds off.
Myth #3: I’ll never be able to enjoy my favorite foods again
After gastric bypass surgery, patients will need to adopt healthier eating habits that support long-term success. While certain foods should be limited, there’s still room to enjoy favorite treats in moderation. The focus after surgery shifts toward mindful portion control, allowing patients to build a balanced, satisfying way of eating for life.
Why choose Loyola Medicine for gastric bypass surgery?
The Center for Metabolic Surgery and Bariatric Care at Loyola Medicine offers many medical and surgical options for weight loss, including gastric bypass surgery. Our team of highly skilled surgeons, medical weight loss doctors, nutritionists and psychologists all draw on research and decades of experience to help every patient lose weight and start living a healthier life.

