Postpartum care: Expert guidance after birth
February 13, 2026
Categories: Obstetrics & Gynecology, Women's Health
A new baby can bring profound joy, but the weeks and months after giving birth can also be a period of significant physical, emotional and hormonal change. For many patients, this time can be especially vulnerable, potentially more so than pregnancy itself. Postpartum care ensures that individuals receive the timely support, monitoring and guidance needed to stay healthy during this important transition.
“The period after childbirth carries a significant risk of complications, yet many can be prevented when patients remain connected to their care teams,” says Maike Liebermann, MD, obstetrics and gynecology specialist.
Why postpartum care matters
Even after an uncomplicated birth, the body goes through major recovery. Health complications can still occur during this time, which is why new individuals should continue to follow the instructions given once they leave the hospital.
While some serious complications can occur during postpartum, most can be identified early and are often preventable with regular follow‑up and support. Staying connected with your care team helps ensure you feel well, recover smoothly and get the help you need if anything feels off.
When to schedule postpartum visits
Two appointments are recommended for you shortly after giving birth.
- First visit: around 2 weeks postpartum
- Second visit: around 6 weeks postpartum
Historically, many patients were only seen at six weeks, but research showed that important complications were being missed. The recommendation now is that all patients have contact with an obstetric provider within the first 3 weeks postpartum, followed by ongoing care and a comprehensive evaluation by 12 weeks.
“These first two appointments don’t need to be their only meetings with doctors. If something feels wrong, do not wait for your scheduled visits to speak with your physician," says Dr. Liebermann.
What happens at the first postpartum visit
Blood pressure monitoring
Blood pressure issues can develop even in people with no prior history. Untreated postpartum hypertension can lead to conditions severe enough to cause stroke or even death.
Symptoms such as severe headaches, vision changes, chest pain, swelling or shortness of breath may signal a hypertensive emergency and require urgent evaluation.
Screening for postpartum depression and anxiety
Postpartum depression and anxiety are common and often under-recognized problems. Hormonal shifts, sleep deprivation and lifestyle changes can contribute to mood disorders. Some individuals feel hesitant to speak up because society expects new parents to be happy.
Postpartum depression can arise anytime in the first year. If you experience persistent sadness, overwhelming anxiety, loss of interest or thoughts of self‑harm, seek care immediately.
C‑section incision check
For those recovering from a cesarean birth, the two‑week visit is essential. Early intervention for infections can prevent more serious complications that might require IV antibiotics or surgical treatment.
What happens at the six‑week postpartum visit
Physical and gynecologic health
This comprehensive visit includes screening for overall health, chronic condition management and recovery from birth‑related injuries or procedures. OB/GYNs ensure patients are up to date on immunizations and Pap smears before they transition back to routine care.
Contraception and pregnancy spacing
Fertility can return sooner than many expect. Short intervals between pregnancies can increase the risk of preterm birth and low birth weight. Discussing contraception helps families plan and reduce risks.
Emotional well‑being
Mental health support remains central throughout postpartum care. Clinicians ensure that individuals have resources for additional evaluation or treatment as needed.
Recognizing postpartum warning signs
Knowing what to expect and watch for can help you seek timely care. Typical recovery can include uterine cramping, breast soreness, fatigue, constipation and increased urination. These symptoms are common as the body heals. But it’s just as important to recognize when something doesn’t feel typical.
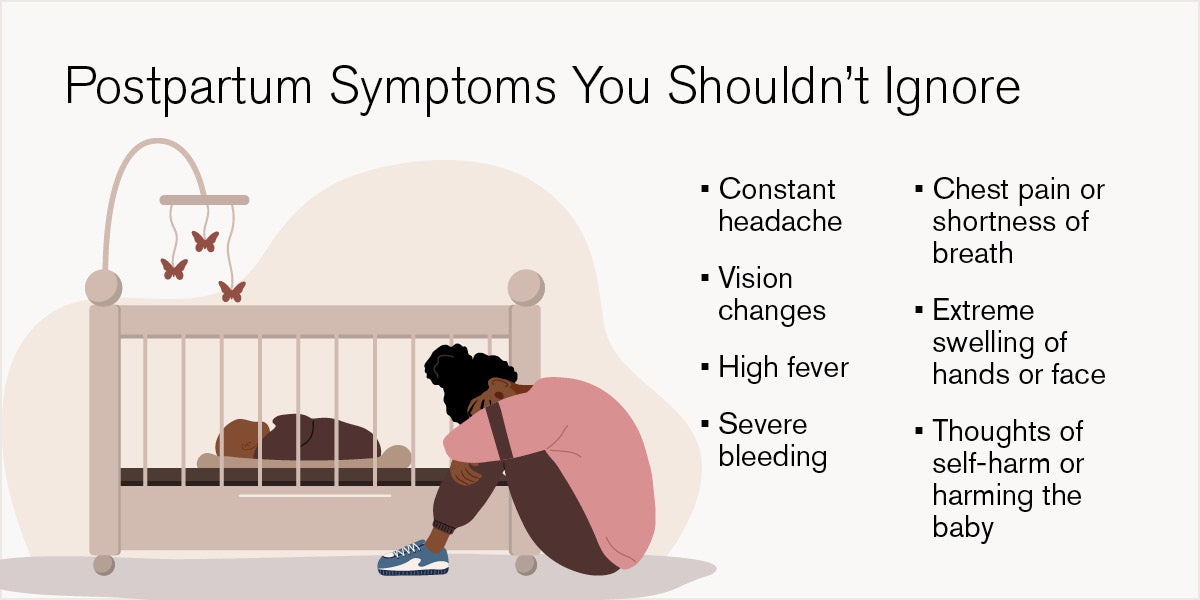
"Even if you aren’t feeling anything serious, a simple thought of ‘something doesn’t feel right’ shouldn’t be ignored,” says Dr. Liebermann. “I’ve had many patients that come to me with an intuition that something is wrong, but they can’t describe it; that’s perfectly fine. Don’t ignore your intuition."
Support between visits
Good communication with your care team is important throughout the postpartum period. Many hospitals schedule follow‑up appointments before discharge to help reduce barriers. Patient portals play a key role, offering:
- Secure messaging for non‑urgent questions
- Responses within about 24 hours from experienced nurses
- Quick escalation to physicians if needed
This allows patients to feel supported in asking questions and seeking guidance between visits.
Breastfeeding and lactation support
Breastfeeding is often portrayed as intuitive, but many families face challenges. Some common issues include:
- Babies feeding unpredictably
- Discomfort difficulty with positioning and latch
- Delays in milk production
Lactation consultants meet with patients shortly after birth to provide hands-on guidance with positioning, latch and feeding techniques. They also set realistic expectations about early feeding patterns and what signs indicate a baby is feeding well. Outpatient lactation support is also available after discharge.
Pelvic floor recovery and physical therapy
Childbirth can weaken pelvic floor muscles, leading to urinary incontinence or pain. Those with higher-grade tears may be referred automatically, but pelvic floor therapy is helpful for anyone experiencing symptoms. A multidisciplinary pelvic floor clinic can support recovery through personalized therapy.
Nutrition and maternal well‑being
Good nutrition is essential but often overlooked in the exhaustion of new parenthood. Irregular sleep and reliance on convenience foods can leave many feeling depleted. Continuing prenatal vitamins during the early postpartum period can help cover basic nutritional needs.
A multidisciplinary approach to postpartum and newborn care at Loyola Medicine
When you’re home adjusting to life with a new baby, it can be harder to stay in touch with your care team. That’s often when unexpected issues come up. The encouraging news is that with regular postpartum check-ins, most complications can be caught early and prevented.
Consistent postpartum visits, awareness of warning signs and open communication with clinicians help ensure a smooth, healthy recovery. Loyola Medicine provides team-based postpartum and newborn care to support families during this period. Newborns typically see their pediatrician within one to three days of discharge, with frequent visits after that. Pediatric teams can also notice signs that a parent may need additional support. This integrated communication helps bridge gaps between obstetric, pediatric and primary care providers.
Our team is here to monitor your recovery, answer questions and help you navigate the physical and emotional changes of early parenthood.
“When patients are home and settling into life with their baby, staying connected can be challenging. Regular postpartum check-ins make a real difference in catching concerns early and preventing complications,” says Dr. Liebermann.

